Stabilizing Spine Treatment
Spinal fusion is a surgical procedure used to strengthen and stabilize areas of the spine affected by injury or degeneration. By permanently joining two or more vertebrae, the surgery reduces painful movement and helps protect nearby nerves from ongoing pressure. This approach is often recommended for conditions that cause structural instability or chronic discomfort. With modern techniques and careful recovery, many patients experience significant improvements in mobility and daily function.
When Spinal Fusion Is Considered
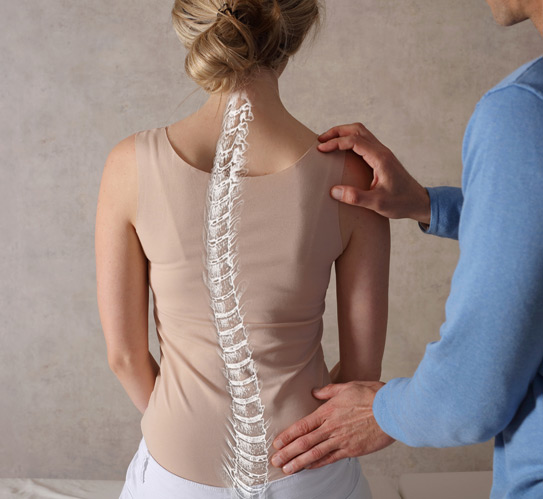
Spinal fusion may be recommended when the spine becomes unstable or when damaged discs can no longer cushion the vertebrae effectively. Conditions such as degenerative disc disease, spondylolisthesis, and spinal fractures commonly lead to painful instability. The procedure can also help correct abnormal spinal curvature in cases of scoliosis. By restoring alignment and reducing movement between vertebrae, spinal fusion aims to relieve nerve compression and prevent further deterioration.
Although fusion can be performed anywhere along the spine, it is most commonly done in the cervical and lumbar regions. Instability from infection, tumors, or traumatic injury may also prompt surgical intervention. Before recommending fusion, orthopedic specialists typically ensure that conservative options like physical therapy, medication, or injections have been fully explored. Patients whose symptoms persist despite these treatments may find that fusion offers meaningful and lasting relief.
How Spinal Fusion Works
Spinal fusion is generally completed in two phases: stabilizing the spine and allowing natural bone growth to complete the fusion. Surgeons begin by removing any damaged disc tissue and placing hardware such as screws, rods, or cages to secure the affected vertebrae. Bone graft material is then applied to promote the formation of solid bone between the vertebrae, creating a permanent connection over time.
Several graft options are available, including the patient’s own bone, donor grafts, or synthetic substitutes designed to encourage new bone formation. The procedure can be performed through the front or back of the spine, depending on the condition being treated. Minimally invasive techniques may be used when appropriate, offering the benefits of smaller incisions, reduced tissue disruption, and potentially faster recovery.
Ideal Candidates for Fusion Surgery
Patients best suited for spinal fusion are those in good overall health without unmanaged medical conditions that could affect healing, such as uncontrolled diabetes or severe hypertension. Non-smokers and individuals within a healthy weight range tend to have higher success rates due to improved circulation and bone healing. A willingness to follow postoperative guidelines, including activity restrictions and physical therapy, also plays a crucial role in recovery. Fusion is typically reserved for patients whose pain or instability persists despite months of conservative treatment.
Recovery and Long-Term Outlook
Healing after spinal fusion takes place gradually as the graft material forms solid bone between the vertebrae. Patients often begin walking shortly after surgery, with physical therapy introduced as healing progresses. Strengthening the surrounding muscles helps support the spine and restore mobility. While full recovery may take several months, many individuals experience reduced pain and improved stability once the fusion matures. With advances in minimally invasive techniques and modern hardware, spinal fusion remains a dependable option for long-term relief from persistent spinal conditions.
