Minimally Invasive Spine Options
Minimally invasive spine surgery is designed to treat spinal conditions using small incisions and precise tools to reduce tissue disruption and shorten recovery time. This approach can help relieve pain from issues such as herniated discs, nerve compression, or instability in the spine. Many patients experience less discomfort and improved mobility when compared with traditional open procedures. With the right surgical plan and follow-up care, minimally invasive spine surgery can support a faster, more comfortable return to daily activities.
How Minimally Invasive Spine Surgery Works
Minimally invasive spine surgery uses advanced imaging, specialized instruments, and smaller incisions to access the spine with minimal disruption to surrounding structures. Surgeons may use mini-open, tubular, or endoscopic techniques depending on the location and type of spinal problem being treated. During the procedure, patients are positioned on the operating table and given either general or local anesthesia for comfort. The use of small surgical channels allows surgeons to reach the affected area without cutting through large sections of muscle.
These techniques help reduce scarring, decrease blood loss, and shorten operative time. Most procedures are completed within a few hours, and incisions are typically closed with stitches or staples. Many patients are able to return home the same day after a brief recovery period. A surgeon will provide detailed post-operative instructions and ongoing monitoring to support healing.
Conditions Treated with Minimally Invasive Techniques
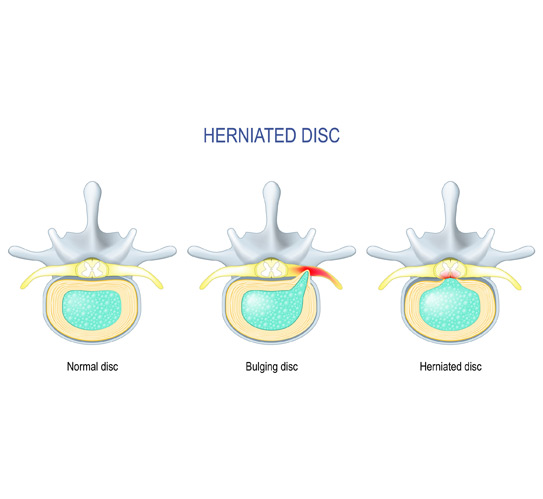
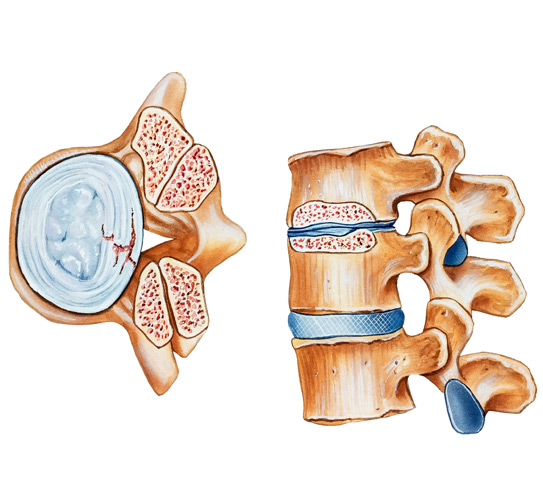
Minimally invasive spine surgery can be used for a range of spinal disorders involving nerve compression, disc damage, or instability. Conditions such as herniated discs, degenerative disc disease, and spinal stenosis may be improved by removing or decompressing affected tissue. MISS may also be used to address certain fractures, infections, or benign spinal tumors that contribute to ongoing pain. Because the procedure limits muscle disruption, many patients see faster improvements in movement and function.
In cases where non-surgical treatments are no longer effective, minimally invasive surgery may offer a more targeted solution. Symptoms such as numbness, tingling, radiating pain, or difficulty standing and walking may indicate that nerve pressure needs to be relieved surgically. A careful evaluation helps determine whether MISS is appropriate and which technique would provide the best outcome.
Benefits of a Minimally Invasive Approach
Minimally invasive spine surgery offers several advantages over traditional open procedures, including reduced muscle damage, lower risk of infection, and decreased post-operative pain. Many patients experience quicker return to normal routines, improved comfort, and shorter rehabilitation periods. Because surrounding tissues are preserved, physical strength often returns more easily, especially when supported by guided physical therapy. These combined benefits allow many individuals to resume daily activities with greater ease.
Candidacy and Treatment Planning
Patients who have persistent spinal pain that does not improve with medication, physical therapy, or lifestyle changes may be good candidates for minimally invasive spine surgery. Those experiencing nerve-related symptoms such as numbness, tingling, or weakness may also benefit from decompression procedures. A thorough assessment, including imaging and a review of non-surgical treatments, helps identify the most effective approach. By partnering with a surgeon experienced in minimally invasive techniques, patients can pursue a plan tailored to their diagnosis, long-term goals, and overall health.
