Understanding Peripheral Neuropathy
Peripheral neuropathy occurs when the nerves that connect the brain and spinal cord to the rest of the body become damaged. These nerves control movement, sensation, and many automatic functions, so damage can lead to pain, numbness, tingling, or weakness—most often in the hands and feet. The condition usually develops gradually and can significantly affect daily comfort and mobility. With proper diagnosis and care, many people can manage symptoms and maintain an active lifestyle.
How Nerve Damage Occurs
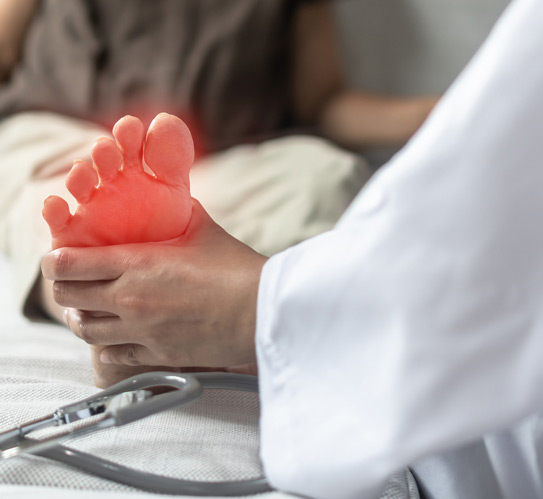
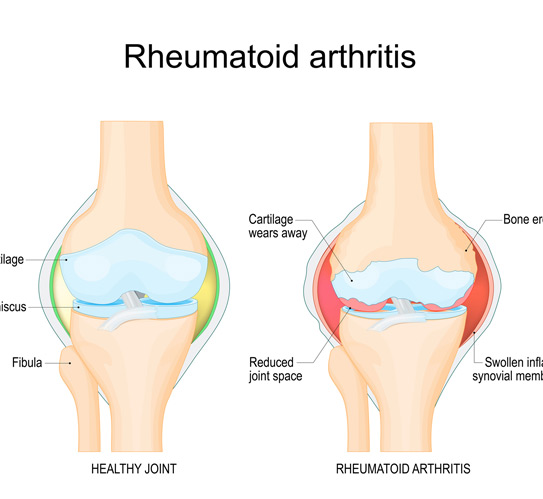
Peripheral nerves can be harmed by a wide range of medical conditions, injuries, and environmental factors. Diabetes is one of the most common causes, with more than half of individuals with type 2 diabetes developing neuropathy. Excessive alcohol use may lead to vitamin deficiencies, which can damage nerve fibers. Autoimmune diseases such as lupus or rheumatoid arthritis can also attack nerve tissue and impair normal function.
Infections—including Lyme disease, shingles, and Epstein-Barr virus—may leave lasting nerve damage even after recovery. Some medications, toxins, and repetitive motions like typing or manual labor also contribute to neuropathy over time. People with kidney, liver, or thyroid disorders, as well as those with a family history of neuropathy, face a higher risk.
Recognizing the Symptoms
Symptoms of peripheral neuropathy typically appear slowly and start with tingling or numbness in the fingers or toes. Pain may feel sharp, burning, stabbing, freezing, or throbbing. Some individuals become extremely sensitive to touch, while others experience weakness or trouble with coordination. If motor nerves are affected, tasks like holding objects, writing, or buttoning clothes may be difficult.
As neuropathy progresses, symptoms may spread and become more disruptive. Some people feel dizzy, struggle with heat intolerance, or develop bladder or bowel issues due to nerve involvement. In severe cases, paralysis or significant loss of sensation can occur, highlighting the importance of early evaluation and treatment.
Treatment and Symptom Relief
Managing peripheral neuropathy often involves addressing both the symptoms and the underlying cause. Pain relievers—from over-the-counter medications to prescription options—can help reduce discomfort. Anti-seizure medications and certain antidepressants are frequently used to calm overactive nerve signals. Topical treatments such as capsaicin creams or lidocaine patches may provide targeted relief. When vitamin deficiencies contribute to nerve damage, supplements can support recovery.
Long-Term Care and Specialized Treatments
More advanced treatments may include transcutaneous electrical nerve stimulation (TENS), immune globulin therapy, or plasma exchange, especially for autoimmune-related neuropathies. Some patients benefit from complementary therapies like acupuncture or chiropractic care. Physical therapy helps restore strength and improve balance if muscle weakness is present. Assistive devices such as braces, canes, or walkers may reduce strain and improve safety during daily activities.
In cases where a nerve is compressed by a growth, scar tissue, or bone spur, surgery may be recommended to relieve pressure and restore function. Ongoing management often involves monitoring underlying conditions, maintaining healthy blood sugar levels, and adopting lifestyle habits that support nerve health. With consistent care and early intervention, many people experience meaningful improvement in their symptoms and quality of life.
