Understanding Tendonitis
Tendonitis is the inflammation or irritation of a tendon—the strong, fibrous tissue that connects muscles to bones. It often develops from repetitive motion, overuse, or sudden injury and can affect nearly any part of the body. Common sites include the shoulders, elbows, wrists, knees, and Achilles tendon. Pain, swelling, and limited movement are typical symptoms, but with early care and proper treatment, most people can recover and return to normal activity.
How Tendonitis Develops
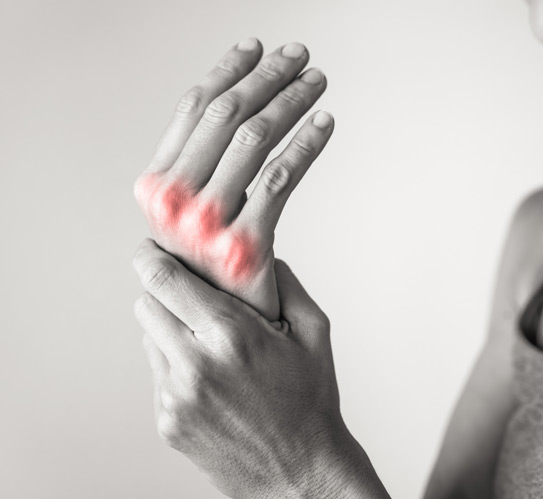
Tendons play a crucial role in movement by transferring force from muscles to bones. When a tendon is subjected to repetitive motion, overuse, or sudden impact, small microtears can form. Over time, these small injuries may lead to inflammation and swelling of the tendon. People who perform repetitive tasks—such as assembly line workers, athletes, or those who frequently use a computer mouse—are at higher risk due to continuous strain on specific tendons.
Underlying health conditions can also contribute to tendonitis. Individuals with osteoarthritis or rheumatoid arthritis may experience biomechanical changes that increase stress on the tendons. Aging is another factor, as tendons gradually lose elasticity and water content, making them more prone to injury. Even a direct blow or fall can cause tendon irritation and inflammation.
Recognizing the Symptoms
Tendonitis symptoms typically involve localized pain and tenderness along the affected tendon. Redness, warmth, and swelling around the area are also common, particularly after periods of rest followed by movement. Many people experience stiffness, especially in the morning or after inactivity, due to inflammation within the tendon sheath. Pain may worsen when contracting the associated muscle or performing repetitive movements.
In more severe cases, tendonitis can limit range of motion or cause significant discomfort during daily activities. Identifying symptoms early helps prevent further irritation and allows for quicker recovery. If pain persists or worsens, medical evaluation can determine whether additional treatment is necessary.
Treatment and Pain Relief
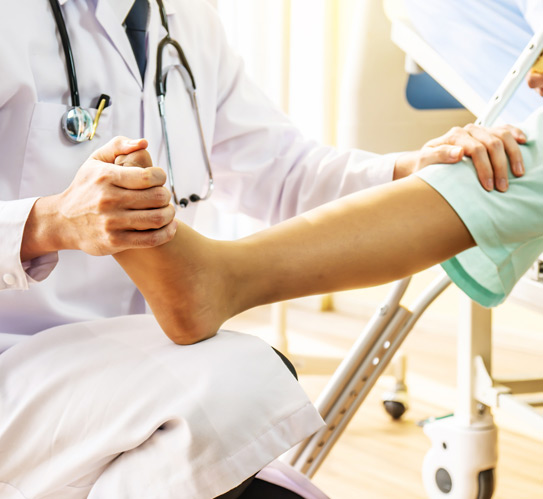
Treatment for tendonitis typically begins with reducing strain on the affected tendon. Rest, ice, compression, and elevation (RICE) are commonly recommended to manage early symptoms. Some physicians use an updated method called POLICE, which incorporates protection and optimal loading rather than full rest, allowing controlled movement to prevent stiffness. Anti-inflammatory medications and corticosteroid injections may be used to ease pain and swelling.
Long-Term Recovery and Prevention
Physical therapy is often an important part of recovery, helping strengthen surrounding muscles and improve flexibility to prevent reinjury. Therapists may recommend stretching exercises, load-management strategies, and techniques to improve posture or movement mechanics. In cases where repetitive activities contribute to tendonitis, modifying work habits, improving ergonomics, or using supportive equipment may help reduce ongoing strain.
With consistent care and proactive management, most people recover fully and return to their usual routines. Following medical guidance, avoiding overuse, and maintaining strong, flexible muscles can significantly reduce the likelihood of tendonitis recurring.
