Understanding Cutting-Edge Injectables
Cutting-edge injectables use concentrated healing components from a patient’s own blood or tissue to support repair in areas affected by injury or inflammation. By delivering these regenerative elements directly to damaged ligaments, tendons, joints, or soft tissues, these treatments aim to reduce pain, improve mobility, and encourage natural healing. Patients may explore this option when conservative care has not provided enough relief, when injuries are slow to recover, or when they want to avoid more invasive procedures.
How Cutting-Edge Injectables Work

These therapies rely on undifferentiated cells—cells that have the ability to adapt and assist in tissue repair. After an evaluation, the clinician collects these cells from the patient, often from fat tissue in the back or hip area. The sample is processed to separate the regenerative components, which are then prepared as an injectable solution.
A local anesthetic is used to numb the injection site, and the concentrated material is delivered into the injured or inflamed area. Treatments are often spaced over several days or weeks, depending on the condition being addressed and how the tissue responds.
Preparing For and Undergoing Treatment
Before treatment begins, the provider performs a thorough assessment, which may include imaging and clinical tests to identify the source of pain or injury. Once collected and prepared, the regenerative material is injected during a short outpatient appointment. Some patients may receive a single injection first to evaluate their response before continuing with a treatment series.
Temporary discomfort or irritation at the injection site may occur, but most side effects are mild. Patients can typically resume normal, non-strenuous activities shortly after the appointment.
When Cutting-Edge Injectables Are Used
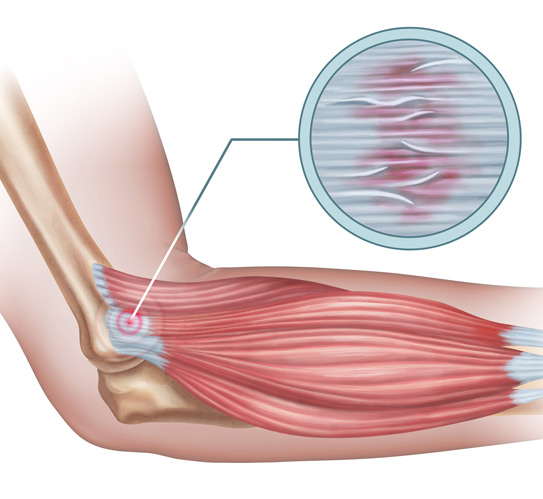
These regenerative treatments may be recommended for patients with slow-healing injuries, chronic joint pain, or degenerative conditions. They are used for non-healing fractures, tendon injuries, partial muscle or ligament tears, and inflammation related to tendinitis or bursitis. Some patients with osteoarthritis may also be candidates, particularly when joint irritation limits movement or contributes to chronic pain.
Because the material is derived from the patient’s own body, this approach is often considered when patients wish to avoid surgery, reduce medication use, or enhance the effectiveness of physical therapy.
Aftercare, Risks, and Guidance
Most patients tolerate the procedure well, with minimal downtime and mild, temporary soreness around the injection site. Serious complications are uncommon, especially because the injected material comes from the patient’s own tissue. Patients should follow their provider’s activity recommendations and may be advised to use targeted physical therapy to maximize results.
Anyone who experiences increasing redness, swelling, fever, or persistent discomfort should contact their provider. With appropriate follow-up and supportive rehabilitation, many individuals experience meaningful improvements in pain, mobility, and daily function.
